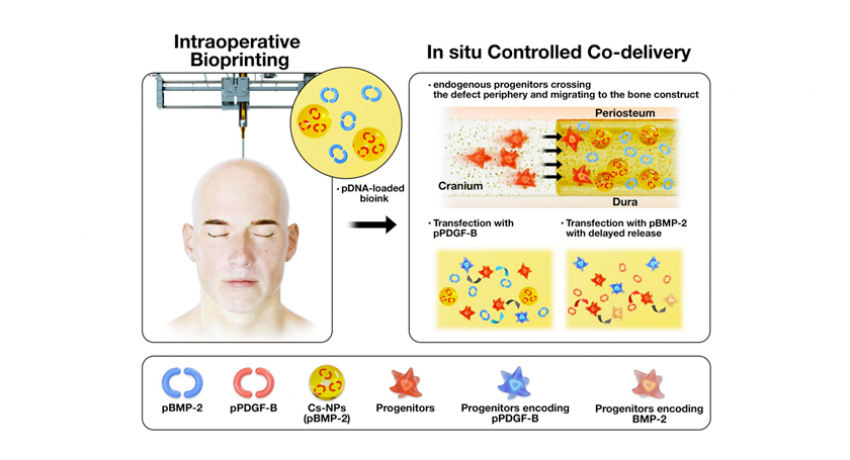
Bioprinting during surgery of bone constructs used as a controlled gene co-delivery platform for the repair of skull defects. Credit: Dong Heo, Kyung Hee University; Ozbolat Lab, Penn State
By A'ndrea Elyse Messer
Given enough time and energy, the body will heal, but when doctors or engineers intervene, the processes do not always proceed as planned because chemicals that control and facilitate the healing process are missing. Now, an international team of engineers is bioprinting bone along with two growth factor encoding genes that help incorporate the cells and heal defects in the skulls of rats.
"Growth factors are essential for cell growth," said Ibrahim T. Ozbolat, associate professor of engineering science and mechanics. "We use two different genes encoding two different growth factors. These growth factors help stem cells to migrate into the defect area and then help the progenitor cells to convert into bone."
The researchers used gene encoding PDGF-B, platelet derived-growth factor, which encourages cells to multiply and to migrate, and gene encoding BMP-2, bone morphogenetic protein, which improves bone regeneration. They delivered both genes using bioprinting.
"We used a controlled co-delivery release of plasmids from a gene-activated matrix to promote bone repair," the researchers stated in the journal Biomaterials.
Ozbolat and his team embedded the DNA for the protein in plasmids — ringlike loops of DNA that can transport genetic information. Once the DNA enters the progenitor cell, it begins to produce the appropriate proteins to enhance bone growth.
The two genes were printed during surgery onto a hole in the skull of a rat using a device very similar to an ink-jet printer. The mixture was created to release a burst of PDGF-B encoding gene in 10 days and a continuing release of BMP-2 encoding gene for five weeks.
The rats that received bioprinted genes with controlled release of BMP-2 encoding gene saw about 40% bone tissue creation and 90% bone coverage in six weeks compared to 10% new bone tissue and 25% bone coverage for rats with the same defect, but no treatment.
"This method is better than simply dumping the growth factors," said Ozbolat. "If we do that, the amounts of proteins are finite, but if we use gene therapy, the cells continue to produce the necessary growth factors."
Working with Ozbolat from Penn State were Kazim K. Moncal, graduate student in engineering science and mechanics; Gregory S. Lewis, assistant professor and Hwabok Wee, postdoctoral fellow both in orthopedics and rehabilitation; Kevin P. Godzik, undergraduate in biomedical engineering: and Elias Rizk, associate professor of neurosurgery.
Others contributing to the research include R. Seda Tigli Aydin, former Penn State postdoctoral fellow now at Bulen Ecevit University, Turkey; Dong N. Heo, former Penn State postdoctoral fellow now at the Kyung Hee University, South Korea; and Timothy M. Acri, former graduate researcher, and Aliasger K. Salem, Lyle and Sharon Bighley Endowed Chair & Professor in Pharmaceutical Sciences, University of Iowa.
The International Team for Implantology, the National Institutes of Health, the National Science Foundation, the Osteology Foundation and the Scientific and Technological Research Council of Turkey supported this work.
Read the full news story here:
https://www.psu.edu/news/research/story/bioprinting-bone-repair-improved-genes